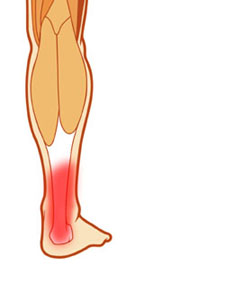
Achilles Tendon Injury
This tendon is named after Achilles, who according to myth was protected from wounds by being dipped in a magical pond by his mother. She held him by the heel, which was not immersed, and later he died by an arrow wound to his heel.
The achilles tendon joins three muscles: the two heads of the gastrocnemius and the soleus. The gastrocnemius heads arise from the posterior portions of the femoral condyles (back of the thigh bone). The soleus arises from the posterior aspect of the tibia and fibula (the two bones in the lower leg).
 The gastrocnemius is a muscle that crosses three joints: the knee, the ankle, and the sub-talar joint (major joint in the foot). The functioning of these joints and influence of other muscles on these joints has a significant effect on the tension that occurs within the achilles tendon. As an example tight hamstrings impact the functioning of the ankle joint, the sub-talar joint, and increase tension in the achilles tendon. The soleus muscle does not cross the knee and is a bi-articular muscle (affects the movement of two joints).
The gastrocnemius is a muscle that crosses three joints: the knee, the ankle, and the sub-talar joint (major joint in the foot). The functioning of these joints and influence of other muscles on these joints has a significant effect on the tension that occurs within the achilles tendon. As an example tight hamstrings impact the functioning of the ankle joint, the sub-talar joint, and increase tension in the achilles tendon. The soleus muscle does not cross the knee and is a bi-articular muscle (affects the movement of two joints).
The bulk of the achilles tendon inserts into the upper back third of the calcaneus (heel bone). Some fibres run further down and insert into the bottom of the heel bone.
Achilles tendinitis develops due to inflammation, strain, or repetitive trauma to the achilles tendon. This occurs usually due to a repetitive activity. Symptoms are also associated with recreational activities like running, tennis and basketball.
If this is left untreated, it can develop into achilles tendinosis, due to a degenerative change in the tendon from repetitive micro-trauma. The tendon scars and the inury becomes chronic in nature.
Causes
Hill running or stair climbing.
Overuse resulting from the natural lack of flexibility in the calf muscles.
Rapidly increasing mileage or speed.
Starting up too quickly after a layoff.
Trauma caused by sudden and/or hard contraction of the calf muscles when putting out extra effort such as in a final sprint.
Tight muscle groups in the back of the leg
Foot type
Two main foot types that can contribute to achilles tendon injury are;
A rigid foot type
A rigid foot causes the foot to spend more time during the running/ walking cycle on the forefoot, this causes the achilles tendon to be used more agressively and for longer throughout the gait cycle. This leads to associated overuse and overpull of the tendon causing injury.
See the video below
A flexible flat foot
A flexible flat foot, sometimes known as a pronated foot can cause excess side to side motion within the shoe this causes a “bowstring” effect putting excess stress on the achilles tendon, leading to injury.
see video below
Tight muscle groups
Tight hamstrings cause the knee to remain flexed during the gait cycle which causes early heel lift at the foot this constant biomechanically stressed position can lead to overpull and subsequent overuse of the achilles tendon.
Tight gastrocnemius causes overpull on the achilles tendon and can lead to injury.
Heel counter on the shoe
The tab at the back of a shoe, particularly a runing shoe can irritate the achilles tendon to such a point that injury can occur. This is particularly the case when the individual has a flexible flat foot type.
Symptoms
Achilles tendinitis often begins with mild pain after exercise or running that gradually worsens.
Other symptoms include:
Recurring localised pain, sometimes severe, along the tendon during or a few hours after running.
Morning tenderness about an inch and a half above the point where the Achilles tendon is attached to the heel bone.
Sluggishness in your leg.
Mild or severe swelling.
Stiffness that generally diminishes as the tendon warms up with use.
Treatment
IF SYMPTOMS PERSISTS OR NUMBNESS/ DISCOLOURATION OF THE FOOT OCCURS CONSULT A MEDICAL PROFESSIONAL IMMEDIATELY.
to restore normal function
As we get older the risk of Achilles tendon rupture goes up dramatically especially if we embark on high impact sporting activities. However it must be emphasised that the risk is still small but when recovering after any injury it is vital that when stretching or performing any exercise that there should be no pain. If any tenderness is elicited then stop and re commence P.R.I.C.E
Prevention
 Remember that virtually all achilles tendon problems occur at contact phase of gait (when the foot hits the ground) due to increased biomechanical stress at this point. No amount of exercising will influence what happens at the point of heel strike, mid-stance and toe off phases of gait. It is therefore vital to improve your biomechanics with orthotics designed for your chosen sport.
Remember that virtually all achilles tendon problems occur at contact phase of gait (when the foot hits the ground) due to increased biomechanical stress at this point. No amount of exercising will influence what happens at the point of heel strike, mid-stance and toe off phases of gait. It is therefore vital to improve your biomechanics with orthotics designed for your chosen sport.
Golden rule- Don’t ignore the problem, it won’t go away!
The way we function biomechanically is predominantly controlled by genetics, its hereditary (runs in the family). The way you function is set and cannot be cured. What you can do however is control lower limb biomechanics by altering foot position during the contact phase of gait. This can only be done by wearing a good shoe (see our shoe guide) and with orthotics (foot beds). This is the cheapest and most cost effective way for any athlete to reduce the risks of injury from occurring and from helping to prevent re-injury. Overall costs for the average athlete will run into pennies per mile/hour of sport. Orthotics are designed to alter the biomechanics during the time the foot is on the ground. They are also used to provide increased shock absorbency working in harmony with the sport shoe worn.
Returning to Activity
The goal of rehabilitation is to return you to your sport or activity as soon as is safely possible. If you return too soon you may worsen your injury, which could lead to permanent damage. Everyone recovers from injury at a different rate. Return to your activity is determined by how soon your achilles recovers, not by how many days or weeks it has been since your injury occurred.
You may safely return to your sport or activity when, starting from the top of the list and progressing to the end, each of the following is true:
You have full range of motion in the injured leg compared to the uninjured leg.
You have full strength of the injured leg compared to the uninjured leg.
You can jog straight ahead without pain or limping.
You can sprint straight ahead without pain or limping.
You can do 45-degree cuts, first at half-speed, then at full-speed.
You can do 20-yard figures-of-eight, first at half-speed, then at full-speed.
You can do 90-degree cuts, first at half-speed, then at full-speed.
You can do 10-yard figures-of-eight, first at half-speed, then at full-speed.
You can jump on both legs without pain and you can jump on the injured leg without pain.